Published: May 2021
Prevention in social care is about encouraging people to be more proactive about their health and wellbeing. It can increase independence and reduce or delay the need for care and support services.
This briefing for local authority commissioners and managers sets prevention in the context of the Care Act and describes the role for commissioners and practitioners, including their distinct responsibilities and the benefits of a shared understanding and approach. It also explores both how prevention is understood in social care and the current evidence base.
Key messages
- The Care Act 2014 highlights prevention as one of seven key responsibilities for local authorities, with an inextricable link to the fundamental principle of promoting wellbeing
- Commissioners and practitioners need to have a shared understanding of the scope of prevention, the different approaches, and the likely opportunities to prevent, reduce or delay need.
- Commissioners need to proactively understand local needs and provision, and to work collaboratively with a wide range of partners.
- Practitioners should take a strengths-based approach and consider at every contact whether a person has needs that can be prevented, reduced or delayed.
- There remains a lack of common understanding and consistency in approach to prevention, which is perhaps unsurprising given the absence of a single definition and the wide range of interventions and objectives.
- There is a clear policy emphasis, which is reflected in regulatory standards, on prevention and promoting independence and wellbeing and this requires a focus on community-centred preventative models of care and support.
- The evidence base for what works remains limited, and the most cost-effective way to use finite resources needs to be judged locally.
What do we mean by prevention in social care?
Prevention, as defined in the Care Act Statutory Guidance (2016), is about the care and support system actively promoting independence and wellbeing. This means intervening early to support individuals, helping people retain their skills and confidence, and preventing need or delaying deterioration wherever possible.
Wistow and Lewis (1997) proposed a two-fold definition of prevention specific to social care, which included the following:
- Services which prevent or delay the need for care in higher-cost, more intensive settings
- Strategies and approaches that promote the quality of life of older people and their engagement with the community.
However, recent analysis of the state of prevention in social care suggests that there is still a lack of common understanding and consistency in the approach to prevention and wellbeing within the social care sector (Skills for Care 2019; Tew et al. 2019; Marczak et al. 2019).
This is perhaps in part because, as the statutory guidance notes, ‘There is no single definition for what constitutes preventative activity’. It ranges from whole-population measures to promote health, to targeted individual interventions to improve functioning for one person. This lack of consensus presents a clear challenge on many levels, for example:
- Which types of services are considered to have preventative effects?
- How do you measure the impact of social care on the prevention agenda?
- How can you agree good practice when you have no common basis of understanding?
Research carried out by Skills for Care in 2019 found that adult social care employers define prevention in four main areas:
- Supporting people to live as healthily as possible, both mentally and physically
- Reducing the use of health services, including primary care, emergency services and hospitals
- Preventing or reducing the escalation of health issues
- Supporting people to remain as independent as possible.
It is also worth considering what the main outcomes for the individual are from prevention, which might be:
- Increased independence, including navigation of prevention and community services and effective self-care
- Improved quality of life and wellbeing for people who need care and support and carers
- Reduced social isolation and loneliness
- Delayed and/or reduced need for care and support.
Prevention – a shared understanding
Given the continued challenge of achieving a common understanding and consistency of approach to prevention, as well as the limited evidence base for what works (see The evidence base), it is helpful that the Care Act guidance provides a framework for commissioners and practitioners, both of whom are well placed to support a focus on prevention. Prevention is often seen as ‘belonging’ to commissioning but true prevention should run all the way through every contact in whatever form it takes. From people using universal services and community groups, to an initial request for information and advice, to assessment, care and support planning, and reviews, and beyond to strategic plans and service development. As the statutory guidance highlights, ‘at every interaction with a person, a local authority should consider whether or how the person’s needs could be reduced or other needs could be delayed from arising’ (DHSC, 2016).
Although there are distinct roles for commissioners and practitioners, if the local authority is to take an effective approach to prevention, there are also some shared responsibilities. Figure 1 below illustrates the joined-up approach to prevention that needs to be taken locally and the role of each partner in an effective system.
Figure 1: Prevention in a joined-up local system
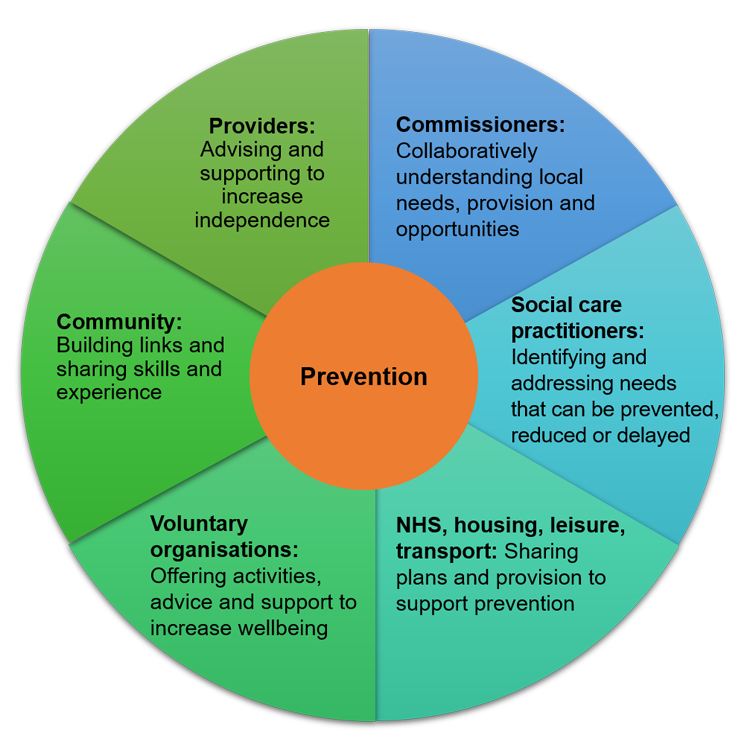
Scope of prevention
Commissioners and practitioners both need to recognise that:
- Prevention isn’t a standalone principle, but one which links closely with wellbeing, empowerment and partnership
- It should be an ongoing consideration, rather than something that happens only once before people develop more significant needs
- The duty to prevent needs from developing or increasing is distinct from the duty to meet eligible needs
- The responsibility applies to all adults:
- Those with no care and support needs
- Those with care and support needs, whether or not those needs are eligible or met by the local authority
- Carers, including those about to take on a caring role, those with no need for support and those whose support needs are not met by the local authority.
Prevention approaches
Both roles also need to understand the three approaches to prevention:
- Prevent – primary prevention/promoting wellbeing
This approach should be applied to everyone, encompassing a range of services, facilities and resources that will help avoid the need for care and support developing. It could include information and advice, promoting healthy and active lifestyles, and reducing loneliness and isolation. - Reduce – secondary prevention/early intervention
This approach is targeted at individuals at risk of developing needs where support may slow this process or prevent other needs from developing. It could include carer support, falls prevention, housing adaptations or support to manage money. - Delay – tertiary prevention/formal intervention
The third approach is aimed at people with established complex health conditions, to minimise the effects, support them to regain skills and to reduce their needs wherever possible. This could include rehabilitation/reablement services, meeting a person’s needs at home, and providing respite care, peer support, emotional support and stress management for carers.
Opportunities for prevention
Both commissioners and practitioners need to be aware of the opportunities for prevention and the importance of providing the right information at the right time. These include:
- Considering the potential opportunities for contact with those who may benefit from preventative support, and where that first contact might be. This may come from an initial contact through the customer services centre, via other professionals (e.g. the GP, community nurse, housing office, or welfare and benefits advisor), or during an assessment of need or carers assessment.
- Using the information and advice service to proactively share information about prevention and preventative services.
- Understanding that although there should be a consistent focus on prevention, there are also some key points at which it may be particularly relevant. These could include bereavement, hospital admission/discharge, going into/out of prison, benefits applications, contact with/use of local support groups, contact with/use of private care and support, and a change in housing.
Commissioner and practitioners can also support a preventative approach by sharing information about available services, future plans, identified needs and unmet needs with one another.
The role for commissioners
The prevention role for the local authority is about facilitating and commissioning services, and working with local organisations to build community capital and make the most of the skills and resources already available in the area. To do this effectively, commissioners need to develop a local plan that outlines how they will meet their duty to prevent, reduce and delay the development of needs in their local population. This plan requires a strategic understanding of local need and provision.
Proactively understanding needs
Commissioners need to consider:
- The number of people who already have care and support needs, or who are at risk of developing needs
- How to identify and target people who fall into these groups
- The level of unmet need
- The needs and aspirations of the local population
Understanding local provision
Planning also requires an accurate picture of what provision already exists and what else is needed:
- What services (including support, universal and community services) already exist that can help prevent, delay and reduce needs, including for carers? Asset-mapping can help with this.
- What mechanisms are needed to identify existing/new services, maintain contact with providers and help people access them?
- What other preventative activity exists (e.g. housing, public health) and how can connections be built?
Commissioners also need to be clear about what the local authority will provide themselves, what can be done in partnership, and what can be most effectively provided by others.
An integrated approach
Prevention is everybody’s business and requires everyone to work together. An effective approach will consider:
- Who else it is important to talk to and work with. This could include public health, leisure, transport, housing, children’s services, NHS, benefits advisors, police, fire service, the voluntary sector, prisons and providers.
- Who to share the assessment of need/unmet need with, in order to develop greater understanding and an integrated approach. It is likely to be particularly important to include independent providers, the NHS (particularly for identifying carers), other agencies and community groups.
The role for frontline social care practitioners
A period of fiscal austerity and rising demand means that local authorities have tended to focus on priority needs. But the recent emphasis from DHSC requires a shift to working in preventative ways and frontline practitioners are well placed to do so at both an individual and community level. They play a key role in promoting independence, enabling people to live the life that they choose, and recognising people’s strengths and the importance of family, friends and communities. These can reduce the risk of health problems and/or delay the need for care and support.
Practitioners now need, at every contact, to consider which needs can be prevented; which could be reduced; which might be delayed; and which need support now.
A preventative approach
In their contact with people, practitioners should take a strengths-based approach and, through genuine conversation, establish a holistic picture of the person’s life. They should look at their strengths, ambitions and priorities; their support networks; their needs and risks; the available community and voluntary groups and resources, and start to answer the question, ‘What does a good life look like for you and how can we work together to achieve it?’.
The conversation should enable the practitioner to establish:
- What is a problem now
- What may become a problem
- What can be done to prevent, reduce or delay the likelihood of those needs developing
The resulting care and support plan should list all the needs that have been identified, whether or not they are eligible, and detail:
- How the person’s eligible needs will be met
- How their non-eligible needs can be addressed to reduce or delay them becoming more significant
Information and advice
Information and advice underpin a shift to more preventative ways of working. Regardless of whether any needs/eligible needs are identified, people should be given information that helps them to prevent/reduce any needs developing, connect with their local community, and delay the onset of greater needs. Information and advice to help in the same way should also be provided to carers.
Information also has a role to play in any preventative measure offered. People are more likely to engage with the support being offered if they understand:
- What needs they have or may develop and why the specific preventative intervention has been suggested
- The difference that it could make
- What will happen when it ends
The policy context
The development of preventative approaches and those which promote independence and wellbeing have gained importance since the implementation of the Care Act 2014.
The NHS Long Term Plan (2019) sets out long-term priorities for better care, quality and outcomes for people who need care and support, and advocates a whole-system approach to prevention, with increased action on prevention and reductions in health inequalities.
Prevention is better than cure (DHSC, 2018) states that:
Prevention is about helping people stay healthy, happy and independent for as long as possible. This means reducing the chances of problems from arising in the first place and, when they do, supporting people to manage them as effectively as possible. Prevention is as important at seventy years old as it is at age seven.
The Government’s consultation green paper Advancing our health: prevention in the 2020s (2019) set out how it plans to embed the vision and tackle the causes of preventable ill health in England.
In 2021, as the adult social care sector starts to look beyond COVID-19 and to recovery, sector leaders agree that it is the opportune time to put preventative approaches to care right at the centre of social care reform.
SCIE says in Beyond COVID (SCIE, 2020) that there is a need to ‘shift investment and focus away from remedial and acute services, towards community-centred preventative models of care, support, housing and technology.
The Local Government Association (LGA) and several social care charities including SCIE signed up to the following principles for future social care reform:
- A person-centred and preventative model of social care, which promotes resilience in local public services and communities
- A commissioning model that creates more person-centred services that help prevent, delay or reduce the need for more formal care services
- A commitment to the Care Act wellbeing principle and to improving people’s choice and control of the care and support they use to live their best life
Regulatory standards
The Care Quality Commission (CQC) promotes working in preventative ways to deliver better outcomes under the ‘effective’ and ‘responsive’ key lines of enquiry. This means that adult social care employers need to take action to ensure that their services meet regulatory standards.
- The CQC Key Lines of Enquiry (KLOEs) set out factors that inspectors assess, including examining how providers support people to live healthier lives (KLOE E4, CQC, 2017).
- The Adult Social Care Outcomes Framework (ASCOF) tool sets priorities for care and measures delayed or reduced need for services.
Prevention in public health and healthcare
The prevention and wellbeing agenda overlaps significantly with integration and the policy drive for closer collaboration between health and social care organisations. This way of working includes strong links with the voluntary and community sector. Closer working relationships can be developed through:
- new care models
- wellbeing teams
- new and emerging job roles
The evidence base
Evidence about what works in prevention remains under-developed so local policy-makers lack information about how best to invest their resources (Allen and Glasby, 2013; Miller and Allen, 2013; Curry, 2006 reported in Marczak et al. 2019). Despite continuing policy expectations that preventative care will deliver cost savings to adult social care and wider systems, formal evidence is neither extensive nor robust.
Marczak (2019) suggests that the limited existing evidence is concentrated on:
- reablement
- telecare
- falls prevention
- community intervention
Evidence of cost-effectiveness is scarce (for exceptions see, for example, Knapp et al., 2010; Henderson et al., 2014; Windle et al., 2009 reported in Marczak et al, 2019; and CPEC/LSE ESSENCE Toolkit, 2019). According to Marczak, assessing cost-effectiveness in prevention is challenging not only due to the lack of a shared understanding of what prevention is, but also because of the difficulties in demonstrating whether it was the interventions that caused the outcomes. Other key challenges in economic evaluations include the long timeframes required for observing the full consequences of preventative investments, the lack of experimental evidence and the challenges involved in disentangling the effects of services and needs (Knapp, 2013; Miller and Allen, 2013 reported in Marczak).
Moreover, Marczak states that the available evidence may not be transferable to unique local contexts and more local evaluations are needed to support judgements about the most cost-effective targeting of limited resources. In summary, the implication of the above literature is that local authorities have relatively few evidence sources to assist them to make informed investment decisions to support their new statutory duty towards prevention. (Marczak et al., 2019)
Skills for Care (Wavehill Social and Economic Research, 2019) summarised the evidence of different approaches as:
- Advice and guidance: evidence from health is promising but there’s no evidence from the social care sector, although uptake of training in this area is growing.
- Physical activity promotion: there’s strong evidence of the impact of promoting exercise and movement, and the role of social care in this work should be further explored.
- Social prescribing: the evidence for social prescribing is inconclusive, however, the number of these schemes is likely to increase which will give a better evidence base for assessing their effectiveness.
- Reablement: there’s evidence to support that reablement improves health-related quality of life and improved service outcomes. Research is ongoing to consider the cost-effectiveness of the approach.
- Asset-based approaches: the complexity of this approach makes forming conclusions from the different types of evidence difficult, but there is potential in developing this approach and our knowledge on the role and impact of social care.
Tew et al. (2019) looked at preventative approaches being implemented in seven local authorities in England and found that ‘second wave’ approaches to prevent, reduce or delay needs for care and support in adult social care in England were often embedded within a variety of strategic initiatives, including:
- Strengths-based models of social work and social care practice (such as Three Conversations)
- Approaches to social networking and building community capacity (such as Local Area Coordination)
- Mobilising the resources of family and personal networks (through approaches such as Family Group Conferencing, peer support or Community Circles)
- Targeted ‘upstream’ use of personal budgets.
What type of services are being commissioned?
Although services specifically focused on prevention are commissioned, many of the activities that help prevent care and support needs from developing or increasing are already available in the local community, entirely separately from adult social care or health. These include:
- Good quality information
- Activities that support safer neighbourhoods
- Group activities that promote healthy, active lifestyles, including exercise classes
- Activities and schemes to reduce loneliness or isolation
Commissioners need to be aware of the range of such opportunities in their area to ensure a broad understanding of and approach to prevention.
Recent research with local authorities suggests that the main types of services commonly trialled included reablement, telecare, adaptations, falls prevention, befriending and community navigators.
Adaptations, telecare, falls preventions and reablement appear to be more commonly commissioned because local or external research is often interpreted as providing evidence of their cost-saving potential. Research suggests that conversely, justifying the commissioning of primary prevention and/or some other community-based services can be more challenging due to perceptions that evidence about their effects was more limited.
Overall, Marczak (2019) suggests the lack of credible data on cost-effectiveness can make it difficult to convince senior management to invest in prevention in a fiscal environment where strategy is driven by budget savings and not policy. However, for reablement, senior managers could draw on resources, such as SCIE’s business case for reablement video (SCIE, 2012) and the economic evidence report produced for the NICE guideline on intermediate care including reablement (Personal Social Services Research Unit. London School of Economics and Political Science, 2017)
Case study: Loneliness
The impact of loneliness and isolation on a person’s physical and mental health, emotional and social wellbeing, relationships and ability to contribute to society makes it a crucial area for prevention under the Care Act.
Commissioners should consider:
- How they can take action on loneliness in their local area, as part of their duty to prevent the development of/increase in care and support needs
- What services, groups and activities exist in their local area that can help prevent and address loneliness and isolation, and how they can be promoted more widely
- What opportunities to identify and act on loneliness may arise from needs assessments and carers assessments, and how practitioners can be supported to offer the right information and advice.
Loneliness, and the links to wellbeing and prevention, is explored in more detail in The Care Act 2014 and loneliness (Campaign to End Loneliness), which includes a link to further guidance:
Practice examples
Sources where you can find practice examples related to preventative approaches being developed and used in adult social care include:
- Innovations in community-centred support (TLAP)
- Prevention is better than cure: case studies (DHSC)
- Community-centred and asset-based approaches (PHE)
- Practice examples (ADASS)
- Case studies (LGA)
- Loneliness Framework (Campaign to End Loneliness)
- Case studies (Bristol Ageing Better)
References
Prevention is better than cure: our vision to help you live well for longer (Department of Health and Social Care, 2018).
Care and support statutory guidance (Department of Health and Social Care, 2016).
ESSENCE Toolkit (London School of Economics and Political Science. Care Policy and Evaluation Centre, 2019)
Marczak J., Wistow G., & Fernandez J-L. (2019). Evaluating social care prevention in England: challenges and opportunities Journal of Long-Term Care, 206–217.
Personal Social Services Research Unit. London School of Economics and Political Science (2017). Intermediate care including reablement, NICE guideline [NG74] Appendix C3: Economic report.
Tew J. et al. (2019). Implementing the Care Act 2014: building social resources to prevent, reduce or delay needs for care and support in adult social care in England Birmingham: University of Birmingham.
Wavehill Social and Economic Research & Skills For Care. (2019). Prevention in social care: where are we now? Leeds: Skills for Care.
