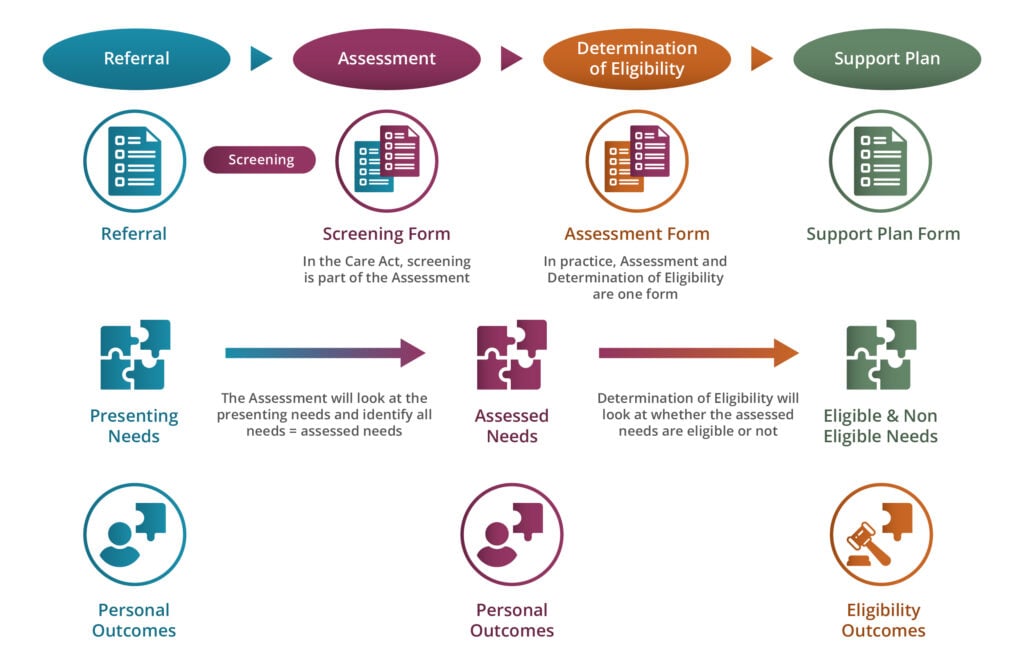
The Care Act 2014 sets out local authorities’ duties when assessing people’s care and support needs.
This resource, updated December 2022, supports care practitioners and answers their questions about assessment and determination of eligibility under the Care Act. It also provides practical guidance over what they should do when applying the letter and spirit of this law.